Investigating New Antibodies To Identify Individuals at Risk of Dengue
Dengue is one of those insidious infections that cause few or no symptoms in the majority of cases – and can therefore spread silently among populations. But of the 50 million cases every year, around 500,000 people contract a particularly severe hemorrhagic form of this “tropical flu”, and 2.5% of them die from the disease.
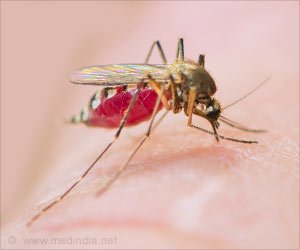
The dengue virus has four different forms, known as serotypes, which are spread by mosquitoes of the Aedes genus in tropical and subtropical countries. Individuals run the risk of being infected by all four serotypes, as if they were catching four different diseases.
Advertisement
“If you are infected with measles, you develop lifelong immunity,” explains lead author Henrik Salje, a statistician and epidemiologist in the Mathematical Modeling of Infectious Diseases Unit at the Institut Pasteur. “But dengue is different. If you are infected by one of the dengue viruses, you become immune to that virus but not to the other three. And those who are infected for a second time by another form of the virus are more likely to develop a severe form of the disease.”
But how can we identify individuals who have already been infected once, and are therefore more at risk than others, if there is every likelihood that they did not suffer any symptoms and fell under the radar of local surveillance networks?
To address this question and try to establish a profile of those most at risk, a group of scientists from the Institut Pasteur, the University of Florida, Walter Reed Army Institute of Research and the University at Buffalo, New York, led by Henrik Salje, decided to investigate the antibodies of individuals and determine thresholds for alert.
“When individuals who have been infected once are infected for a second time by another form of the dengue virus, their antibody levels increase, but not enough to protect them,” explains Henrik Salje. “It’s as if the antibodies cling to the virus but are unable to neutralize it.”
“These individuals fall within a significant “window of risk”; they are at high risk of developing hemorrhagic dengue,” continues Simon Cauchemez, last author of the paper and Head of the Mathematical Modeling of Infectious Diseases Unit.
To determine the boundaries of this “window of risk”, the scientists decided to take a fresh look at detailed data from a cohort of Thai patients recruited between 1998 and 2003 by researchers at the University at Buffalo and Walter Reed. For the purposes of the study they developed a bespoke mathematical and statistical model.
The cohort data concerns 3,451 children from a rural region in northern Thailand. They were given a blood test every 90 days for 5 years, so the scientists were able to observe their antibody levels over time. The children were also closely monitored to see whether they experienced dengue symptoms.
All data were fed into the model developed by the team and, after performing a sophisticated statistical analysis, the scientists were able to determine antibody levels associated with a higher risk of complication.
“This analysis identified the context and level of antibodies that place a given individual within the “window of risk” – meaning that these people can immediately be monitored more closely,” sums up Henrik Salje.
“Characterization of individual risks offers the promise that we can monitor populations in the same way, and determine when a population might be collectively at risk of experiencing high rates of dengue disease,” adds Derek Cummings, co-author of the study and Professor of Biology at the University of Florida.
“The study also emphasized the difficulties involved in establishing an effective vaccine strategy for dengue, since the existing vaccines do not offer full protection against all serotypes,” reveals Simon Cauchemez.
These findings advance our understanding of the virus and offer new prospects for identifying individuals who would benefit from closer monitoring and vaccination.
Source: Eurekalert
Source link
#Investigating #Antibodies #Identify #Individuals #Risk #Dengue



