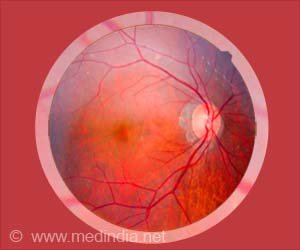
Diabetic Retinopathy Can Worsen With Low Blood Sugar Levels
The study, which involved human and mouse eye cells and intact retinas produced in a low sugar (low glucose) environment in the laboratory, as well as mice with low glucose levels, was published in
.
“Temporary episodes of low glucose happen once or twice a day in people with insulin-dependent diabetes and often among people newly diagnosed with the condition,” says Akrit Sodhi, M.D., Ph.D., the Branna and Irving Sisenwein Professor of Ophthalmology at the Wilmer Eye Institute at Johns Hopkins Medicine. Low glucose levels can also occur during sleep in people with non-insulin-dependent diabetes. “Our results show that these periodic low glucose levels cause an increase in certain retinal cell proteins, resulting in an overgrowth of blood vessels and worsening diabetic eye disease,” adds Sodhi.
Diabetes-related eye disease is one of the most avoidable causes of blindness in the United States. Diabetic retinopathy, which affects up to one-third of diabetics, is defined by the abnormal development of blood vessels in the retina.
According to Sodhi, the new study implies that persons with diabetic retinopathy may be especially vulnerable to low glucose levels and that maintaining stable glucose levels should be an important aspect of glucose control.
Advertisement
The researchers examined protein levels in human and mouse retinal cells and whole retinas grown in a low-glucose environment in the laboratory, as well as in animals with intermittent low blood sugar.
How Low Glucose Levels Damage the Eye?
Low glucose levels in human and animal retinal cells generated a cascade of molecular alterations that can lead to blood vessel enlargement, according to the researchers. First, the researchers discovered that low glucose levels reduced retinal cells’ ability to break down glucose for energy.
The researchers discovered that when they looked specifically at Müller glial cells, which are supportive cells for neurons in the retina and rely primarily on glucose for energy production, the cells increased the expression of the GLUT1 gene, which produces a protein that transports glucose into cells.
The researchers discovered that when cells were exposed to low glucose levels, they boosted the amounts of a transcription factor known as a hypoxia-inducible factor (HIF)-1. This activated the cellular machinery required to improve their ability to utilize available glucose, saving the minimal oxygen available for energy production by retinal neurons (including GLUT1).
However, in low-oxygen situations, such as those found in diabetic eye disease patients’ retinas, this normal, physiologic response to low glucose caused a flood of HIF-1 protein into the cell’s nucleus, the cell’s control center.
This increased the synthesis of proteins like VEGF and ANGPTL4, which stimulate the formation of aberrant, leaky blood vessels – the primary cause of vision loss in diabetic eye disease patients.
The researchers intend to investigate if low glucose levels in diabetics affect comparable molecular pathways in other organs such as the kidney and brain.
According to Sodhi, the HIF-1 pathway could be a useful target for creating new therapeutics for diabetic eye disease.
Source: Medindia
Source link
#Diabetic #Retinopathy #Worsen #Blood #Sugar #Levels



